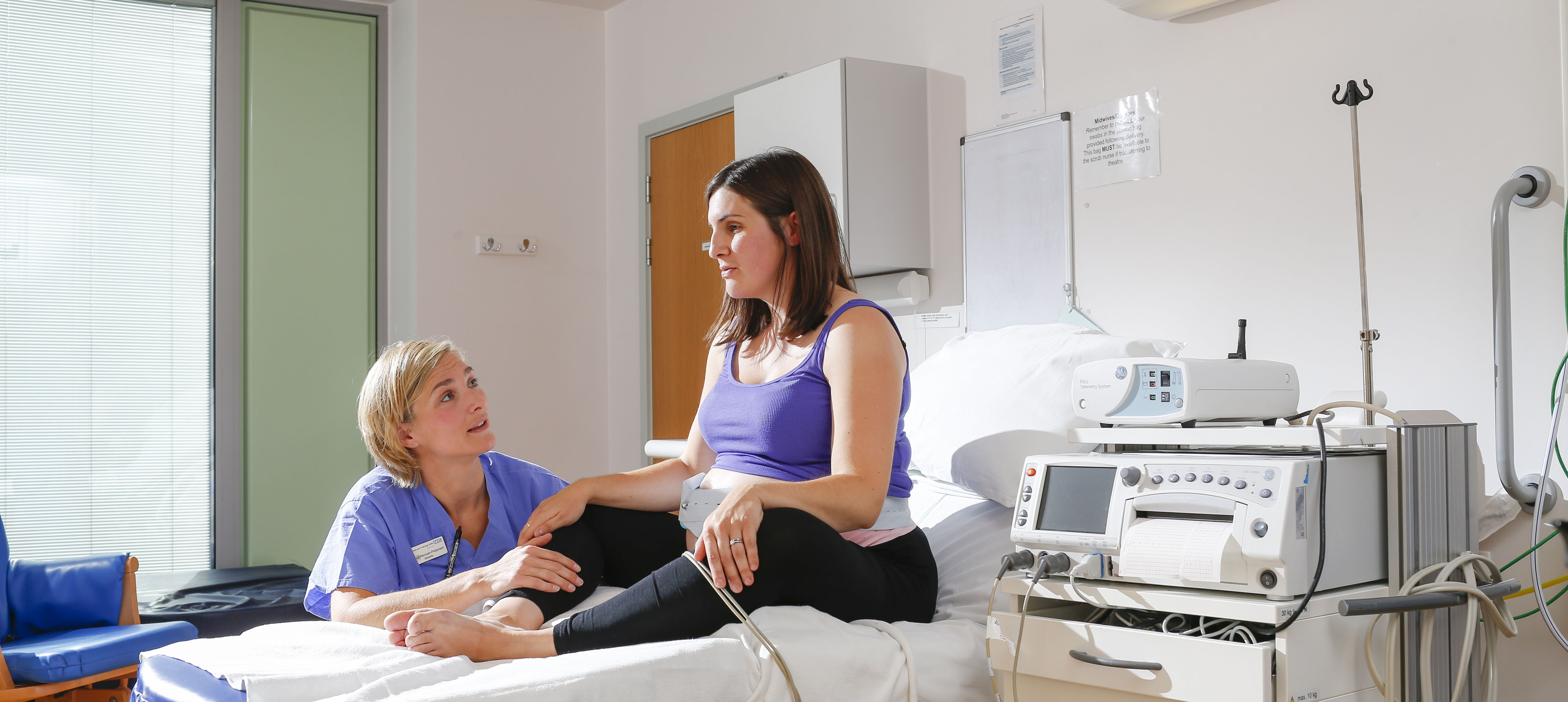
Pregnancy appointments
You will mainly be under the care of a midwifery team throughout your pregnancy. Most women/pregnant people should have a named midwife who will oversee your pregnancy care. You may also require the care of a Doctor if your pregnancy is deemed more complex or you have pre-existing health conditions.
During an appointment with your midwife, they will check the health of you and your baby, give you useful information and answer any questions.
Your schedule of appointments will vary depending on your individual circumstances and this will be discussed with you, with your midwife, at the initial appointment. If you’re pregnant with your first baby, you’ll have more appointments than those already with children. See more about pregnancy appointments here.
At Maidstone and Tunbridge Wells NHS Trust we follow the Perinatal Institute Gap and Grow Growth Assessment Protocol, this will be discussed with you on an individual basis.
Non-pregnancy related care will still be provided by your GP or specialist team.
The Health Visiting team will also be in contact with you towards the end of your pregnancy and once your baby is born to continue your community care.
Below is more information on some of the appointments you will be invited to:
8-10 weeks of pregnancy - booking
Most see a midwife by 10 weeks of pregnancy. This first appointment is called a ‘booking appointment’ and the midwife will take your history and give you your pregnancy information. You may wish to take a look at the following leaflets and information on choosing where to have your baby before your appointment.
The community midwife will:
- Review:
- Medical history including details of medications, date of last smear test and plan of care
- Your mental health history
- Obstetric history, if applicable – your previous pregnancies including dates, complications, baby weights (you may wish to bring the red personal child health record book)
- Any social/safeguarding history including your social workers name and contact details
- Family medical history
- Any relevant medical/mental health/social/safeguarding history of your partner/baby’s father
- Ensure your dating scan and combined screening are booked if you would like these tests. More information on screening tests in pregnancy can be found here
- Check your blood pressure
- Record your weight, height and body mass index
- Make any necessary referrals to hospital or other specialist services
- Offer carbon monoxide screening
- Discuss your personalised antenatal care and support plan
- Complete your personal hand held maternity records which are kept by you and in which all of the care you receive during your pregnancy will be documented
- Answer any questions, thoughts or feelings you may have about this or any previous pregnancy
11-14 weeks of pregnancy - dating/combined screening ultrasound scan
The dating/combined ultrasound scan is usually offered at around 11 to 14 weeks. It is quick and takes only about 20 minutes. The purpose of this scan is to measure the size of your baby to accurately confirm the due date. This scan can also be used, in combination with a blood test, to assess the likelihood of your pregnancy being affected by Down’s Syndrome and other chromosomal abnormalities.
For more information on screening tests for you and your baby visit our Screening in Pregnancy page.
16 weeks of pregnancy
Your midwife or doctor will give you information about the ultrasound scan you’ll be offered at 18 to 20 weeks.
They’ll also help with any concerns or questions you have.
Your midwife or doctor should:
- Give you a booklet called Building a Happy Baby and have a short discussion on the importance of noticing and responding to you your baby’s movement when they start at approximately 20 weeks’
- review, discuss and record the results of any screening test
- measure your blood pressure and test your urine for protein
- consider an iron supplement if you’re anaemic
18–21 weeks of pregnancy - anomaly scan
The anomaly (abnormality) scan is performed at around 18 – 20+6 weeks of pregnancy. This will provide a detailed examination to check the baby is developing normally. We also check your baby’s growth, the position of the placenta and the amount of fluid around the baby.
Occasionally it is not possible to obtain all the views of baby and a second scan will be offered to complete the anomaly scan by 23 weeks. If the scan shows a possible problem, you will be referred to a specialist to confirm findings and where necessary discuss the options available to you. It is important to remember that not all abnormalities will be detected on ultrasound scan.
28 weeks of pregnancy
Your midwife or doctor should:
- use a tape measure to measure the size of your uterus
- measure your blood pressure and test your urine for protein
- offer more screening tests
At 28 weeks of pregnancy we routinely offer to test your blood to check your iron levels. You may need to take iron supplements during your pregnancy to keep your Haemoglobin (iron) at the desired level for birth. More information about Vitamins in pregnancy can be found here.
If you have a Rhesus negative blood group, your midwife will discuss this with you. More information about Anti-D can be found here.
34-38 weeks of pregnancy
Your midwife or doctor should:
- review, discuss and record the results of any screening tests from the last appointment
- use a tape measure to measure the size of your uterus
- measure your blood pressure and test your urine for protein
- have a short discussion about feeding, comforting and caring for your baby and the importance of this for your baby’s brain development
During your pregnancy you would have been asked to think about where you may want to give birth. At Maidstone and Tunbridge Wells NHS Trust you have the options of homebirth, birth in a Birth Centre and birth in a Hospital. Towards the end of your pregnancy your midwife will go over your pregnancy to help you decide where you will be suitable to have your baby. More information about your choices can be found here.
This appointment is an opportunity to talk about your wishes for labour and birth, including pain relief, Vitamin K for your baby and infant feeding. You may find it helpful to take a look at our Infographics for Labour and Birth Choices. For more information about the ways in which you can enhance your labour and birth, please visit our Birth Optimising page.