
Tunbridge Wells Hospital is the first Level 2 neonatal unit in the world to recruit to an important study aiming to improve outcomes for babies with brain injuries at birth.
Eliza, born in October last year, was the first baby to be recruited to a research study at Tunbridge Wells Hospital aiming to improve care for babies who suffer from brain injury at birth.
Shortly after baby Eliza’s birth, her parents, Casey and Ryan, were told she may have mild hypoxic ischaemic encephalopathy (HIE) after staff noticed rapid breathing and a delay in Eliza’s reflexes.
Mild HIE is a type of brain injury that occurs when a baby experiences lack of oxygen at birth and affects around 0.5 to 1 in every 1,000 newborns. Though traditionally considered low risk, recent research shows many affected infants face lasting cognitive and neurological challenges, and around 20% may develop lifelong disability such as cerebral palsy.
Dr Kudzai Mugweni, Consultant Paediatrician at Maidstone and Tunbridge Wells NHS Trust (MTW), quickly made the new parents aware of the COMET (Cooling in Mild Encephalopathy Trial) study.
Run by doctors and researchers from Imperial College London and funded by the National Institute for Health and Care Research, the COMET study is examining if cooling therapy can reduce brain injury in babies who have experienced HIE.
The study involves using a special cooling blanket or mattress which can reduce brain injury, assessing how well it can help to prevent later disability. This carefully lowers a baby’s temperature from the normal temperature of 37ºC to a temperature of 33.5ºC for the first three days after birth.
The neonatal unit at Tunbridge Wells Hospital is the first of its kind in the world to recruit to the COMET study. Tunbridge Wells Neonatal Unit is a Level 2 unit, which means it provides specialised care for premature or sick babies needing high dependency care.
“We made the decision to go ahead with the trial very quickly. Dr Mugweni explained everything clearly in a way we could understand, so we could carefully think about the possible benefits and risks. After considering everything, we decided it was definitely worth trying,” said Eliza’s parents.
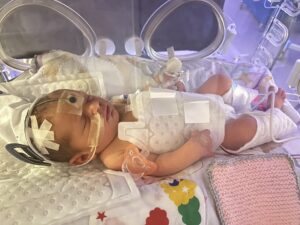 Eliza was quickly transferred from the Neonatal Intensive Care Unit at Tunbridge Wells Hospital to the Level 3 Neonatal Intensive Care Unit at Medway Maritime Hospital to continue her cooling treatment.
Eliza was quickly transferred from the Neonatal Intensive Care Unit at Tunbridge Wells Hospital to the Level 3 Neonatal Intensive Care Unit at Medway Maritime Hospital to continue her cooling treatment.
“It was difficult spending time away from Eliza in her first few days of life, but we knew she was being taken care of and the doctors could see she was responding well,” said Casey.
Eliza is now doing well and achieving all her developmental milestones and is having regular physiotherapy and occupational therapy monitoring. She will have check-ups at Tunbridge Wells Hospital, before being invited to Imperial College London to check on her development.
“For any parents considering taking part in the COMET study, I’d say the short-term pain of losing out on time with your newborn baby is difficult, but worth it for the potential long-term benefits of the treatment,” said Eliza’s father, Ryan.
Dr Mugweni said: “For too long, a mild HIE diagnosis was seen as low risk, often resulting in a wait and see approach. By leading Imperial’s COMET study at Tunbridge Wells Hospital, we are helping to transform that mindset – shifting care from passive observation to proactive protection, so every baby we treat has the brightest, healthiest future possible.”
MTW’s Paediatric Research team works with families of the Trust’s youngest patients to explore opportunities to participate in research studies.
Liz Day, Neonatal Research Nurse, said: “Research gives families access to the most up to date developments in care, and studies like COMET help us find better ways to protect babies who have had a difficult start in life. Every family who takes part helps to shape the future of care for newborns.”
Professor Sudhin Thayyil, the lead investigator of the study based at Imperial College London, said: “Every year, around 1,000 babies in the UK suffer sudden, unexpected brain injuries, even after healthy pregnancies. Developing better treatments is incredibly challenging. Doctors have just hours after birth to carefully assess tiny, vulnerable babies and their brain activity using special tests, explain the study sensitively to exhausted parents, obtain consent, and deliver treatment under intense pressure.
“Every moment counts, and every breakthrough could transform a baby’s life. That is why it is vital for every hospital in the NHS to take part in these studies so that all babies have the best possible start and parents can make informed choices, no matter where their child is born.”