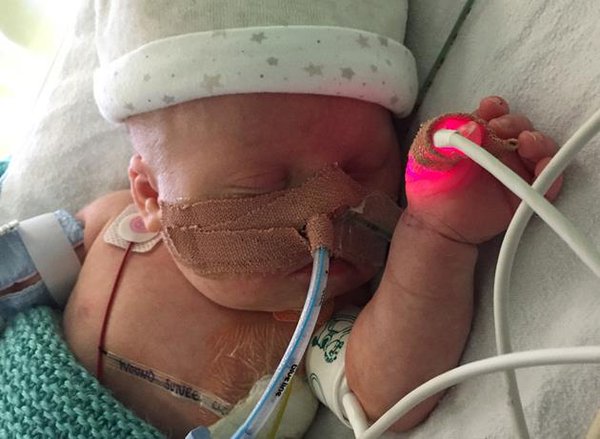
Fergus Ainsworth was born three weeks early on 1 February 2016. Having previously been diagnosed with Down’s Syndrome, Fergus’s parents, Julius and Sinead Ainsworth, were prepared for the challenges that lay ahead, however, nothing could have prepared them for what happened one week after Fergus’ birth, when he was rushed to Tunbridge Wells Hospital.
Here is his story …
Fergus, who is Julius and Sinead’s third child, was diagnosed with Down’s Syndrome following the routine 12 week scan. At 30 weeks, it was discovered that he also had a small ventricular septal defect (VSD), meaning he had a hole in the wall that separates the left and right ventricles of the heart. The remainder of Sinead’s pregnancy proceeded uneventfully, during which she received excellent antenatal care at Maidstone Hospital and the Evelina London Children’s Hospital.
On 31 January, Sinead went into labour three weeks early and delivered Fergus naturally at Tunbridge Wells Hospital the following day. She and Fergus remained in hospital for three days before they headed home to Fergus’s very excited brother and sister, ready to settle back into daily life.
Sinead said, “On the evening of Saturday 6 February, I noticed that Fergus had become unresponsive and I was struggling to rouse him. He was beginning to feel cool and I couldn’t obtain a reading on the thermometer when trying to take his temperature. Recognising that there was a serious problem, and fearing the worst, Julius and I rushed him straight to A&E at Tunbridge Wells Hospital.”
On arrival, doctors immediately began Fergus’ examination. As they went through the routine questions with Sinead and Julius, they immediately summoned specialists to attend to Fergus’ varied and urgent needs.
Dr Sarah Sharp, the anaesthetic registrar, arrived and proceeded to get a line into Fergus, while warming him with a hypothermic blanket. Dr Sharp provided essential breathing support until the consultant anaesthetist, Dr Jamie Goodman, and the consultant paediatrician, Dr Nikila Pandya, arrived to intubate Fergus, whose heart rate and blood pressure were dangerously low.
Once he was stabilised, ventilated, had an IV line in and was wrapped in an insulation blanket, Fergus was taken to theatre for x-rays. It was established that there was fluid on his left lung, which explained his difficulty breathing. In essence, Fergus was drowning.
Sinead remembers: “It was awful seeing him like that, such a tiny bundle all wrapped up, and we didn’t know what to expect. It was so surreal, a real out of body experience.”
The South Thames Retrieval Service collected Fergus the following morning and transported him to the Evelina London Children’s Hospital where he was admitted to the Paediatric Intensive Care Unit (PICU).
Following a scan of his heart, a drain was inserted into Fergus’ left lung to commence draining of the fluid and lines were inserted into him to administer medication required to improve his vital signs.
That week, all Fergus’ tests for potential infections and viruses came back negative. He had CT scans, brain scans and bowel scans, all of which indicated nothing untoward, however, by this stage his right lung also began showing signs of a build up of fluid around it. Another drain was inserted, this time on his right side. It was then discovered that the fluid draining from his chest also contained chyle, leading to a diagnosis of an extremely rare condition known as Congenital Bilateral Chylothorax, which results from lymph fluid leaking from the thoracic duct. While this condition is very rare, there is an increased incidence in children with Down’s Syndrome.
Fergus continued to improve, but a CAT scan indicated a build up of air in the pleural space around the lung. Urgent treatment ensued to remove the air and stabilise his lung function.
Julius said: “The next target was to get Fergus off the ventilator and breathing independently. This took five days with Fergus initially doing well, but due to his slow progress, he was put on continuous positive air pressure (CPAP) to help support his breathing and enable this to continue.”
The cardiology team involved in Fergus’ care performed an echo scan of his heart which showed that his VSD (hole in his heart) was now considered to be of moderate size. The team treated this with medication at first, to allow Fergus to gain weight and get stronger. However, a week later he had already reached the maximum dosage of medication allowed for his size and weight and his breathing had not improved. This meant that ultimately a heart operation was inevitable.
On the day Fergus turned five weeks old he had open heart surgery. The entire procedure lasted five hours, with the actual operation lasting one hour.
A week after the operation, following a routine echo scan, an incompetent valve was discovered in his heart, meaning that Fergus could not be completely signed off by the cardiac team at that point. This would require further monitoring, but as his lungs grew stronger the leak began to diminish.
Two weeks after the operation, the cardiology team signed him off and he was handed over to the respiratory team and transferred from the Paediatric Intensive Care Unit (PICU) to the High Dependency Unit (HDU).
Ten days later the family finally got the all clear and Fergus was discharged from hospital. The two-month ordeal was nearing an end and Fergus was coming home!
Sinead and Julius said: “We are eternally grateful to everyone who helped with Fergus during what was a really difficult time. We received nothing but the most caring, selfless and professional lifesaving NHS treatment – and it all started over a weekend. If it weren’t for the amazing staff on duty that weekend, he would not have survived.
“The wonderful staff at the Evelina London Children’s Hospital treated him and nursed him back to health, but the fast and thoughtful actions of the staff at Pembury Hospital undoubtedly saved his life.”
They added: “When we look back now and think of all that the teams did for us, we feel so humbled and grateful. We were powerless and had to put our trust in the doctors. It was hard, but their expertise, knowledge and overall unfailing dedication and care saved our son.”